
INHIBRX Investor Presentation Innovation Driven Outcomes Focused

2 Presentation disclaimer This presentation of Inhibrx Biosciences, Inc. (the “Company”) contains forward-looking statements. In some cases, you can identify forward-looking statements by the words “will,” “expect,” “intend,” “plan,” “objective,” “believe,” “estimate,” “potential,” “continue” and “ongoing,” or the negative of these terms, or other comparable terminology intended to identify statements about the future. These statements are based on management’s current beliefs and expectations. These statements include but are not limited to statements regarding the Company’s business strategy, the Company’s plans to develop and commercialize its product candidates, the safety and efficacy of the Company’s product candidates, the Company’s plans and expected timing with respect to clinical trials and regulatory filings and approvals, manufacturing matters, strength of intellectual property protection, and the size and growth potential of the markets for the Company’s product candidates, and any implication that pre- clinical data or preliminary or topline results will be representative of the results of later trials. This presentation also contains certain projections and estimates regarding the Company’s future financial performance, namely potential future revenue for certain of the Company’s product candidates. This information also constitutes forward-looking information and is for illustrative purposes only and should not be relied upon as necessarily being indicative of any future results. The assumptions and estimates underlying this estimated financial information are inherently uncertain and subject to a wide variety of significant business, economic competitive and other risks and uncertainties that could cause actual results to differ materially from those contained in the prospective financial information. These potential financial information and other forward- looking statements involve substantial known and unknown risks, uncertainties and other factors that may cause the Company’s actual results, levels of activity, performance or achievements to be materially different from the information expressed or implied by these forward-looking statements. Additional information regarding the Company’s risks and uncertainties are described from time to time in the “Risk Factors” section of our Securities and Exchange Commission filings, including those described in our Annual Report on Form 10-K as well as our Quarterly Reports on Form 10-Q, and supplemented from time to time by our Current Reports on Form 8-K. The Company may not actually achieve the plans, intentions or expectations disclosed in its forward-looking statements, and you should not place undue reliance on the Company’s forward-looking statements. Actual results or events could differ materially from the plans, intentions and expectations disclosed in the forward-looking statements the Company makes. The forward- looking statements in this presentation represent the Company’s views as of the date of this presentation. The Company anticipates that subsequent events and developments will cause its views to change. However, while the Company may elect to update these forward-looking statements at some point in the future, the Company has no current intention of doing so except to the extent required by applicable law. You should, therefore, not rely on these forward-looking statements as representing the Company’s views as of any date subsequent to the date of this presentation. The investigational product candidates discussed in this presentation have not been approved or licensed by the U.S. Food and Drug Administration or by any other regulatory authority, and they are not commercially available in any market. This presentation also contains estimates and other statistical data made by independent parties and by the Company relating to market size and growth and other data about its industry. This data involves a number of assumptions and limitations, and you are cautioned not to give undue weight to such estimates. In addition, projections, assumptions, and estimates of the Company’s future performance and the future performance of the markets in which it operates are necessarily subject to a high degree of uncertainty and risk. The Inhibrx logo is a registered trademark of Inhibrx Biosciences, Inc. All third-party trademarks used herein are registered trademarks of their respective owners. This presentation shall not constitute an offer to sell or the solicitation of an offer to buy securities.
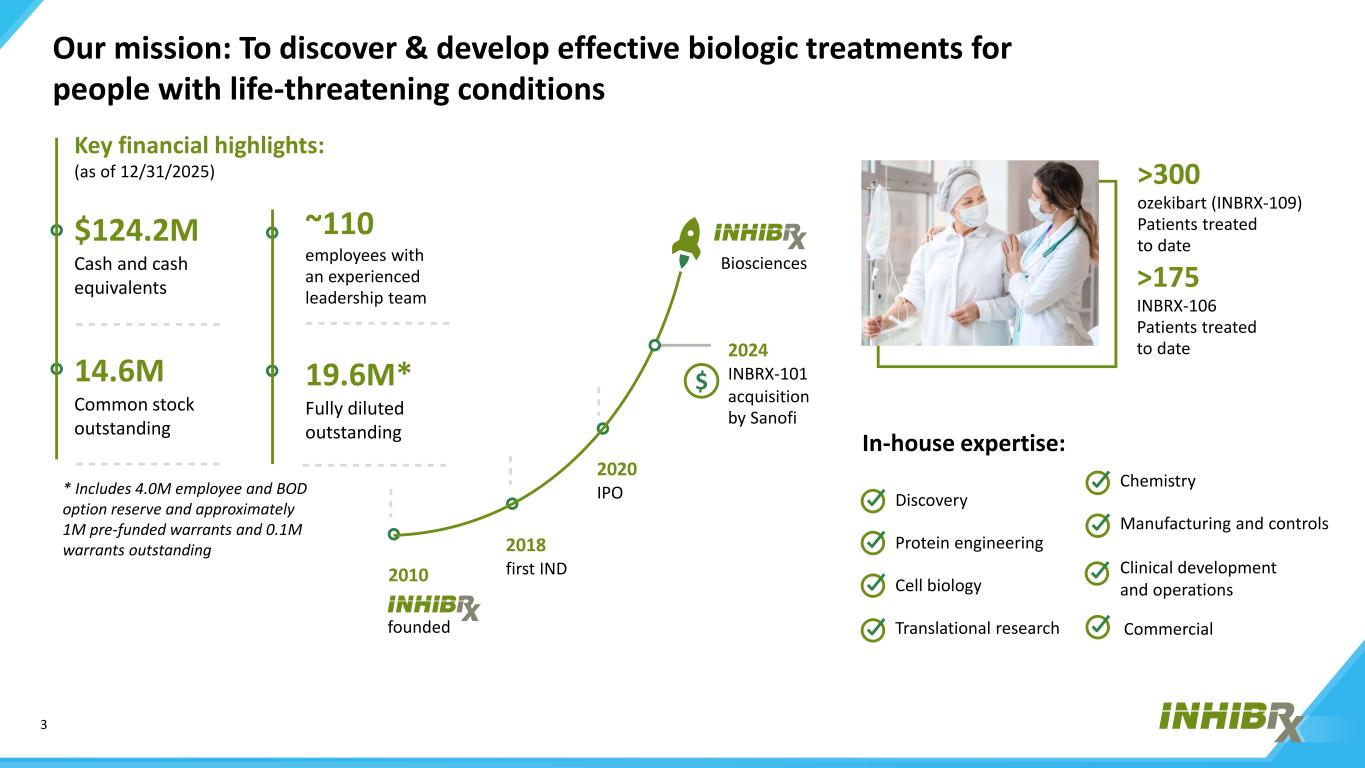
3 $ Biosciences founded 2018 first IND 2020 IPO 2024 INBRX-101 acquisition by Sanofi 2010 >300 ozekibart (INBRX-109) Patients treated to date >175 INBRX-106 Patients treated to date Our mission: To discover & develop effective biologic treatments for people with life-threatening conditions ~110 employees with an experienced leadership team Key financial highlights: (as of 12/31/2025) $124.2M Cash and cash equivalents 14.6M Common stock outstanding 19.6M* Fully diluted outstanding In-house expertise: Discovery Protein engineering Cell biology Translational research Chemistry Manufacturing and controls Clinical development and operations Commercial * Includes 4.0M employee and BOD option reserve and approximately 1M pre-funded warrants and 0.1M warrants outstanding
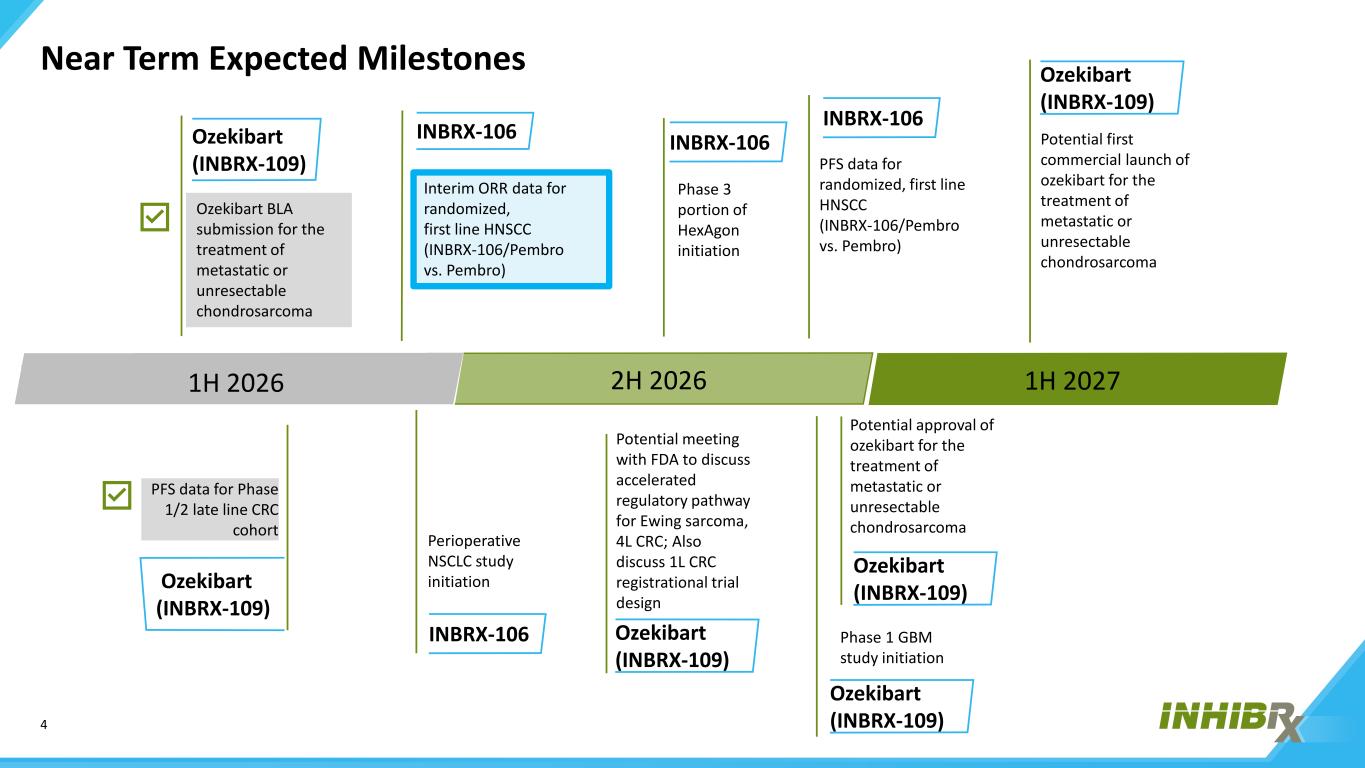
4 Near Term Expected Milestones 1H 2026 INBRX-106 Interim ORR data for randomized, first line HNSCC (INBRX-106/Pembro vs. Pembro) 2H 2026 Ozekibart BLA submission for the treatment of metastatic or unresectable chondrosarcoma Ozekibart (INBRX-109) Ozekibart (INBRX-109) PFS data for Phase 1/2 late line CRC cohort INBRX-106 PFS data for randomized, first line HNSCC (INBRX-106/Pembro vs. Pembro) Ozekibart (INBRX-109) Potential approval of ozekibart for the treatment of metastatic or unresectable chondrosarcoma Potential meeting with FDA to discuss accelerated regulatory pathway for Ewing sarcoma, 4L CRC; Also discuss 1L CRC registrational trial design Ozekibart (INBRX-109) INBRX-106 Phase 3 portion of HexAgon initiation INBRX-106 Perioperative NSCLC study initiation 1H 2027 Ozekibart (INBRX-109) Potential first commercial launch of ozekibart for the treatment of metastatic or unresectable chondrosarcoma Phase 1 GBM study initiation Ozekibart (INBRX-109)

INBRX-106 Boosting PD-1 efficacy through next-generation hexavalent OX40 agonism
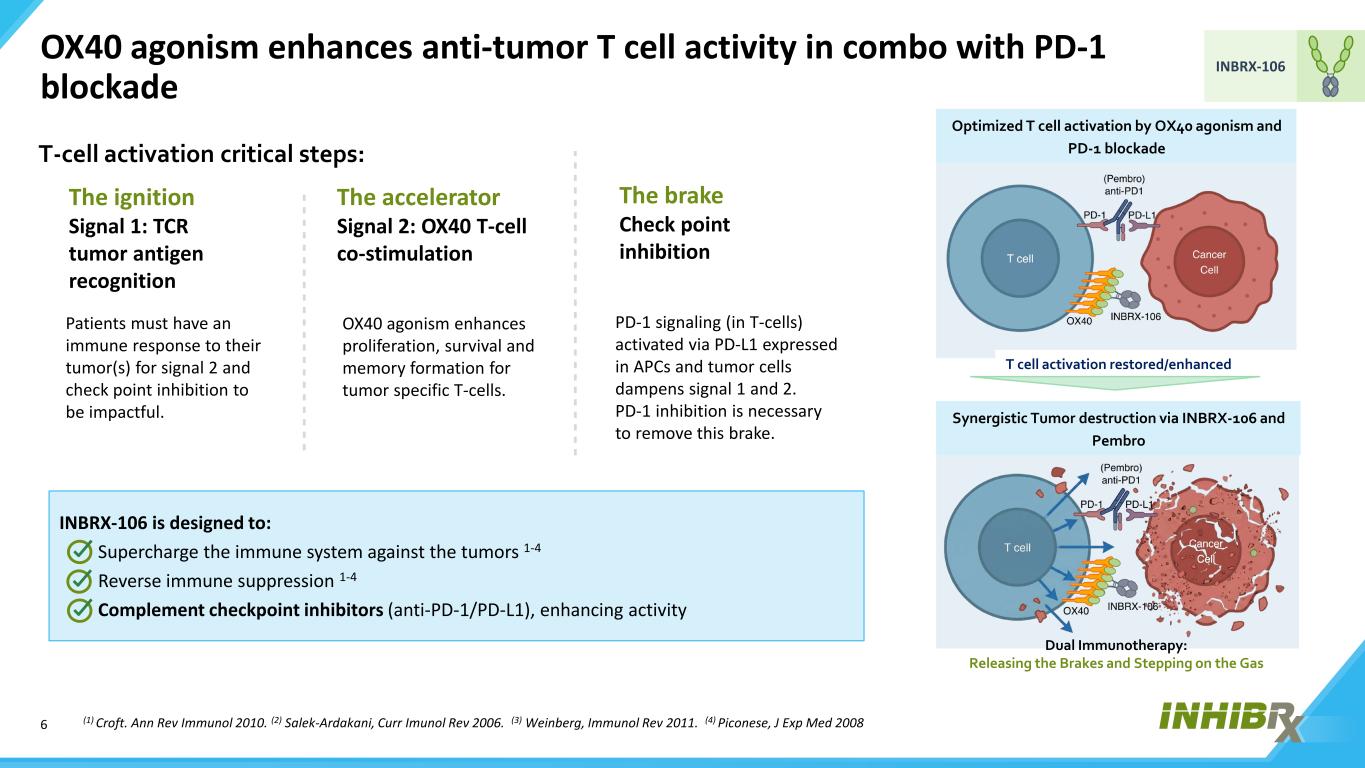
6 INBRX-106 OX40 agonism enhances anti-tumor T cell activity in combo with PD-1 blockade (1) Croft. Ann Rev Immunol 2010. (2) Salek-Ardakani, Curr Imunol Rev 2006. (3) Weinberg, Immunol Rev 2011. (4) Piconese, J Exp Med 2008 T cell activation restored/enhanced Optimized T cell activation by OX40 agonism and PD-1 blockade Dual Immunotherapy: Releasing the Brakes and Stepping on the Gas Synergistic Tumor destruction via INBRX-106 and Pembro INBRX-106 is designed to: Supercharge the immune system against the tumors 1-4 Reverse immune suppression 1-4 Complement checkpoint inhibitors (anti-PD-1/PD-L1), enhancing activity Patients must have an immune response to their tumor(s) for signal 2 and check point inhibition to be impactful. T-cell activation critical steps: The ignition Signal 1: TCR tumor antigen recognition OX40 agonism enhances proliferation, survival and memory formation for tumor specific T-cells. PD-1 signaling (in T-cells) activated via PD-L1 expressed in APCs and tumor cells dampens signal 1 and 2. PD-1 inhibition is necessary to remove this brake. The accelerator Signal 2: OX40 T-cell co-stimulation The brake Check point inhibition
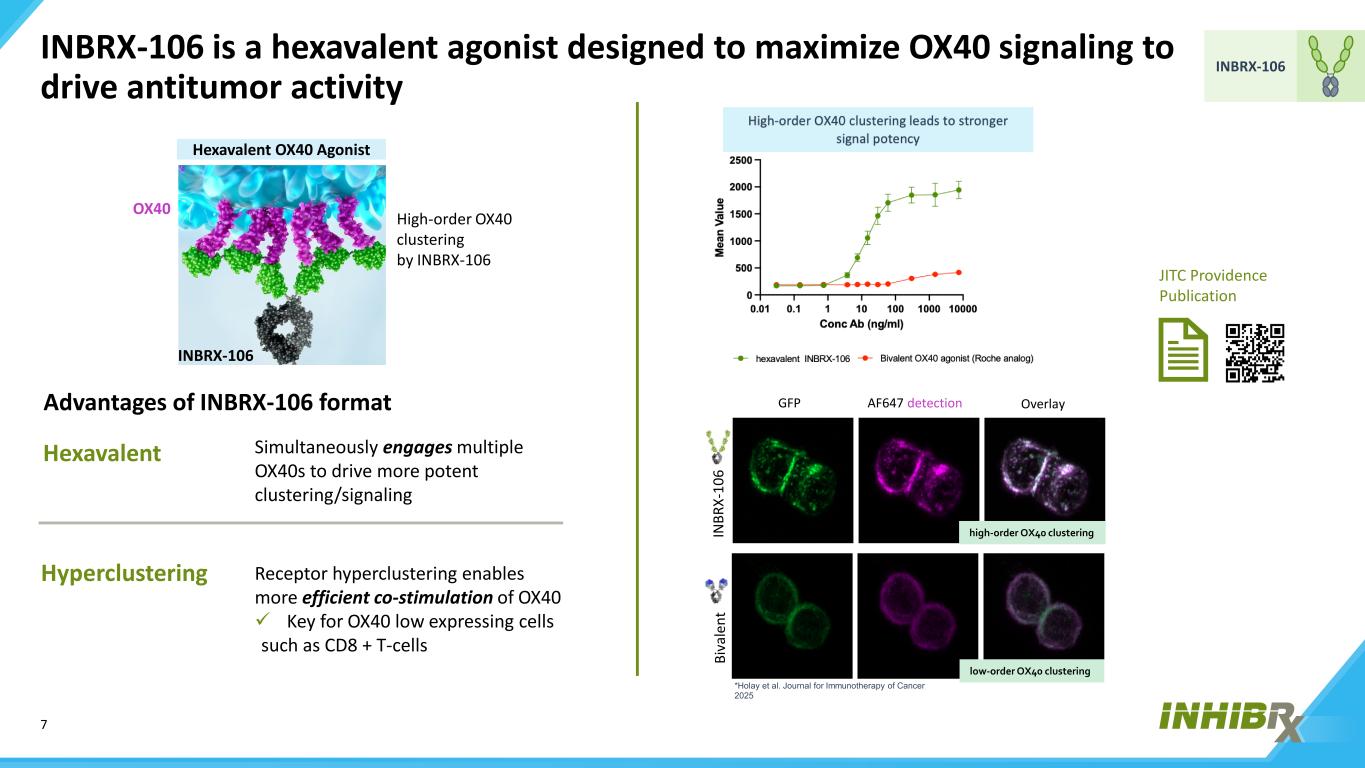
7 INBRX-106 INBRX-106 is a hexavalent agonist designed to maximize OX40 signaling to drive antitumor activity IN BR X- 10 6 Bi va le nt AF647 detection OverlayGFP high-order OX40 clustering low-order OX40 clustering *Holay et al. Journal for Immunotherapy of Cancer 2025 Advantages of INBRX-106 format Hyperclustering Hexavalent Simultaneously engages multiple OX40s to drive more potent clustering/signaling Receptor hyperclustering enables more efficient co-stimulation of OX40 Key for OX40 low expressing cells such as CD8 + T-cells Hexavalent OX40 Agonist OX40 INBRX-106 High-order OX40 clustering by INBRX-106 JITC Providence Publication
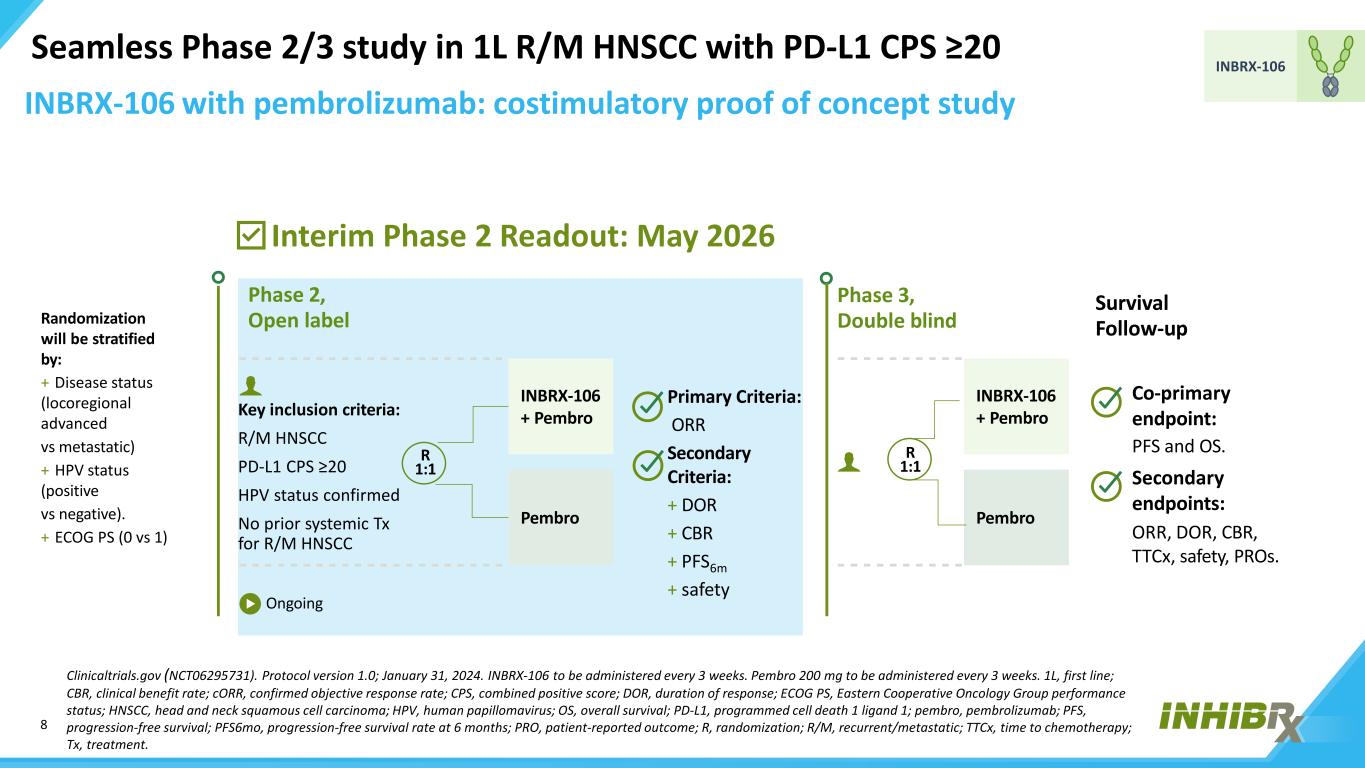
8 INBRX-106 Seamless Phase 2/3 study in 1L R/M HNSCC with PD-L1 CPS ≥20 Clinicaltrials.gov (NCT06295731). Protocol version 1.0; January 31, 2024. INBRX-106 to be administered every 3 weeks. Pembro 200 mg to be administered every 3 weeks. 1L, first line; CBR, clinical benefit rate; cORR, confirmed objective response rate; CPS, combined positive score; DOR, duration of response; ECOG PS, Eastern Cooperative Oncology Group performance status; HNSCC, head and neck squamous cell carcinoma; HPV, human papillomavirus; OS, overall survival; PD-L1, programmed cell death 1 ligand 1; pembro, pembrolizumab; PFS, progression-free survival; PFS6mo, progression-free survival rate at 6 months; PRO, patient-reported outcome; R, randomization; R/M, recurrent/metastatic; TTCx, time to chemotherapy; Tx, treatment. Randomization will be stratified by: + Disease status (locoregional advanced vs metastatic) + HPV status (positive vs negative). + ECOG PS (0 vs 1) Phase 2, Open label Phase 3, Double blind Survival Follow-up Ongoing INBRX-106 + Pembro INBRX-106 + Pembro Pembro Pembro Co-primary endpoint: PFS and OS. Secondary endpoints: ORR, DOR, CBR, TTCx, safety, PROs. Primary Criteria: ORR Secondary Criteria: + DOR + CBR + PFS6m + safety Key inclusion criteria: R/M HNSCC PD-L1 CPS ≥20 HPV status confirmed No prior systemic Tx for R/M HNSCC R 1:1 R 1:1 Interim Phase 2 Readout: May 2026 INBRX-106 with pembrolizumab: costimulatory proof of concept study
9 INBRX-106 Interim HexAgon Phase 2 data in 1L HNSCC demonstrate INBRX-106 Potential costimulatory benefit over PD-1 monotherapy Improvement in cORR with superior depth of response Confirmed objective response rate (cORR): • 44.0% with INBRX-106 + pembro • 21.4% with pembro alone Superior depth of response: • 3 complete radiographic response (CRs) in INBRX-106 + pembro; no CRs observed in pembro alone • Deeper tumor reductions overall in INBRX-106 + pembro arm, with majority of responding patients achieving >50% target lesion shrinkage Pharmacodynamic evidence of potent T-Cell co-activation Increased T-Cell expansion: • Up to 15-fold mean increase in proliferation of CD8+ and CD4+ T- Cells vs. pembro alone • Up to 4-fold mean increase in activation of CD8+ and CD4+ T-Cells vs. pembro alone Consistent with the expected mechanism of action of INBRX-106 as a potent T-cell costimulator Manageable safety profile consistent with immunotherapy combination INBRX-106 + pembro demonstrated generally manageable safety profile, consistent with the addition of an active immunostimulatory agent to checkpoint blockade Data support initiation of INBRX-106 Phase 3 HexAgon (1L HNSCC) expected in 3Q 2026 and expansion into additional settings such as perioperative NSCLC and 1L metastatic NSCLC
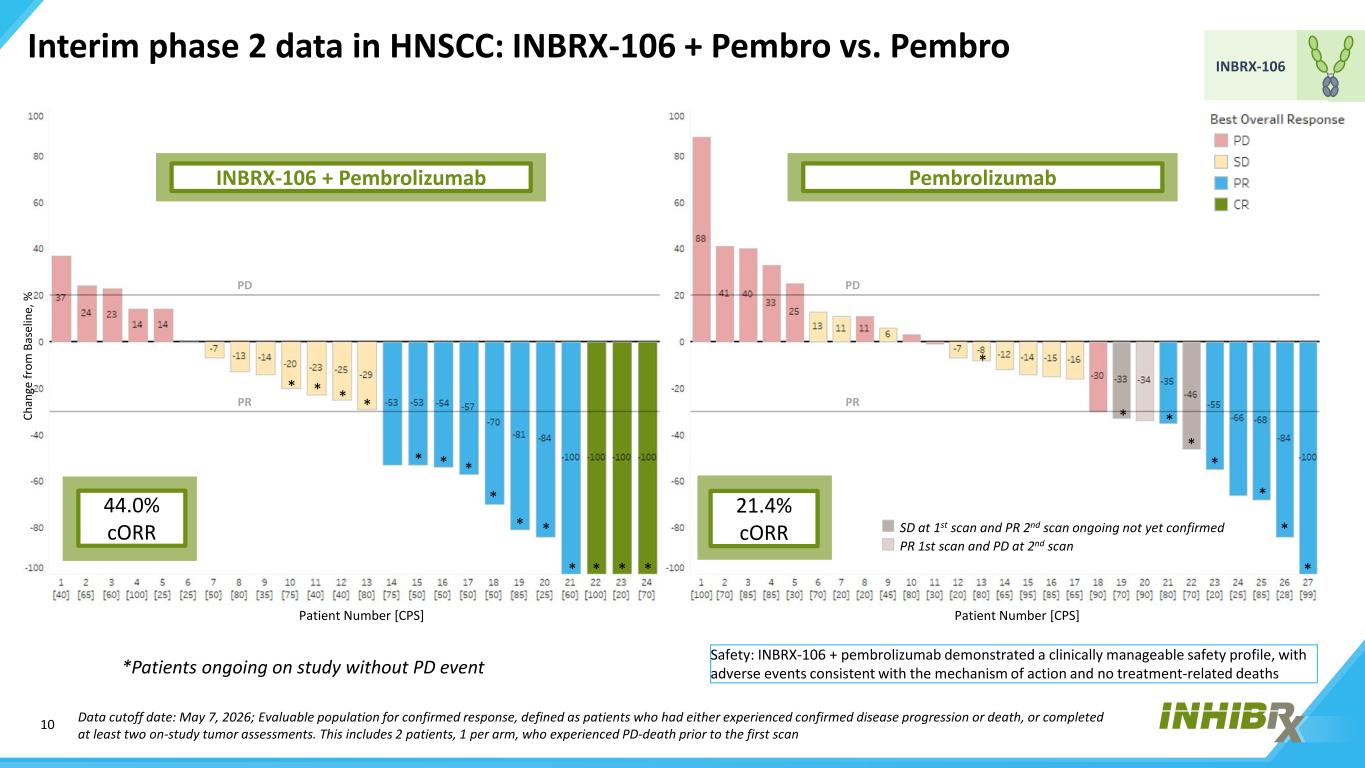
10 INBRX-106 SD at 1st scan and PR 2nd scan ongoing not yet confirmed PR 1st scan and PD at 2nd scan 44.0% cORR Patient Number [CPS] Patient Number [CPS] 21.4% cORR INBRX-106 + Pembrolizumab Pembrolizumab Interim phase 2 data in HNSCC: INBRX-106 + Pembro vs. Pembro Ch an ge fr om B as el in e, % PR PD PR PD Safety: INBRX-106 + pembrolizumab demonstrated a clinically manageable safety profile, with adverse events consistent with the mechanism of action and no treatment-related deaths Data cutoff date: May 7, 2026; Evaluable population for confirmed response, defined as patients who had either experienced confirmed disease progression or death, or completed at least two on-study tumor assessments. This includes 2 patients, 1 per arm, who experienced PD-death prior to the first scan ** * * *Patients ongoing on study without PD event * * * * * * * * * * * * * * * * * *
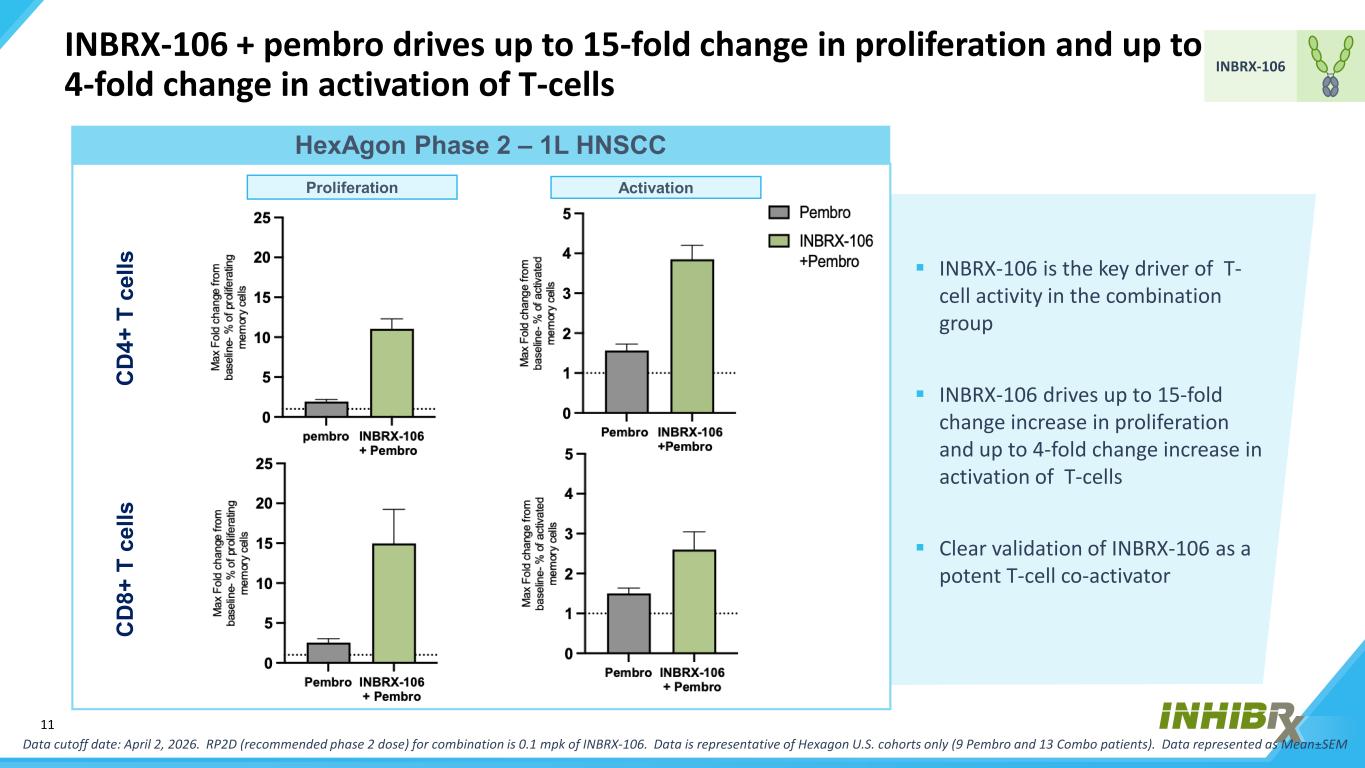
11 INBRX-106 INBRX-106 is the key driver of T- cell activity in the combination group INBRX-106 drives up to 15-fold change increase in proliferation and up to 4-fold change increase in activation of T-cells Clear validation of INBRX-106 as a potent T-cell co-activator Data cutoff date: April 2, 2026. RP2D (recommended phase 2 dose) for combination is 0.1 mpk of INBRX-106. Data is representative of Hexagon U.S. cohorts only (9 Pembro and 13 Combo patients). Data represented as Mean±SEM HexAgon Phase 2 – 1L HNSCC Proliferation Activation C D 4+ T c el ls C D 8+ T c el ls INBRX-106 + pembro drives up to 15-fold change in proliferation and up to 4-fold change in activation of T-cells
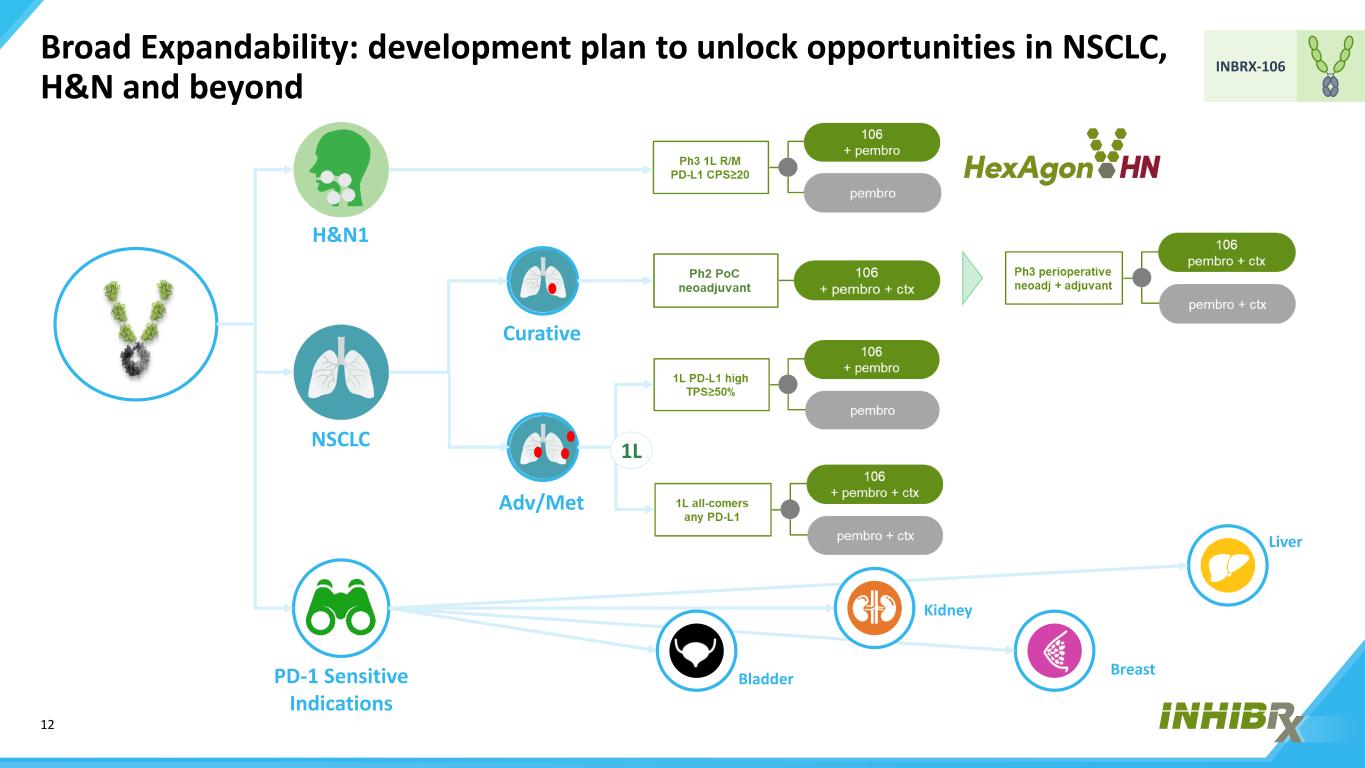
12 INBRX-106 Broad Expandability: development plan to unlock opportunities in NSCLC, H&N and beyond H&N1 NSCLC PD-1 Sensitive Indications Adv/Met Curative 1L Bladder Kidney Breast Liver
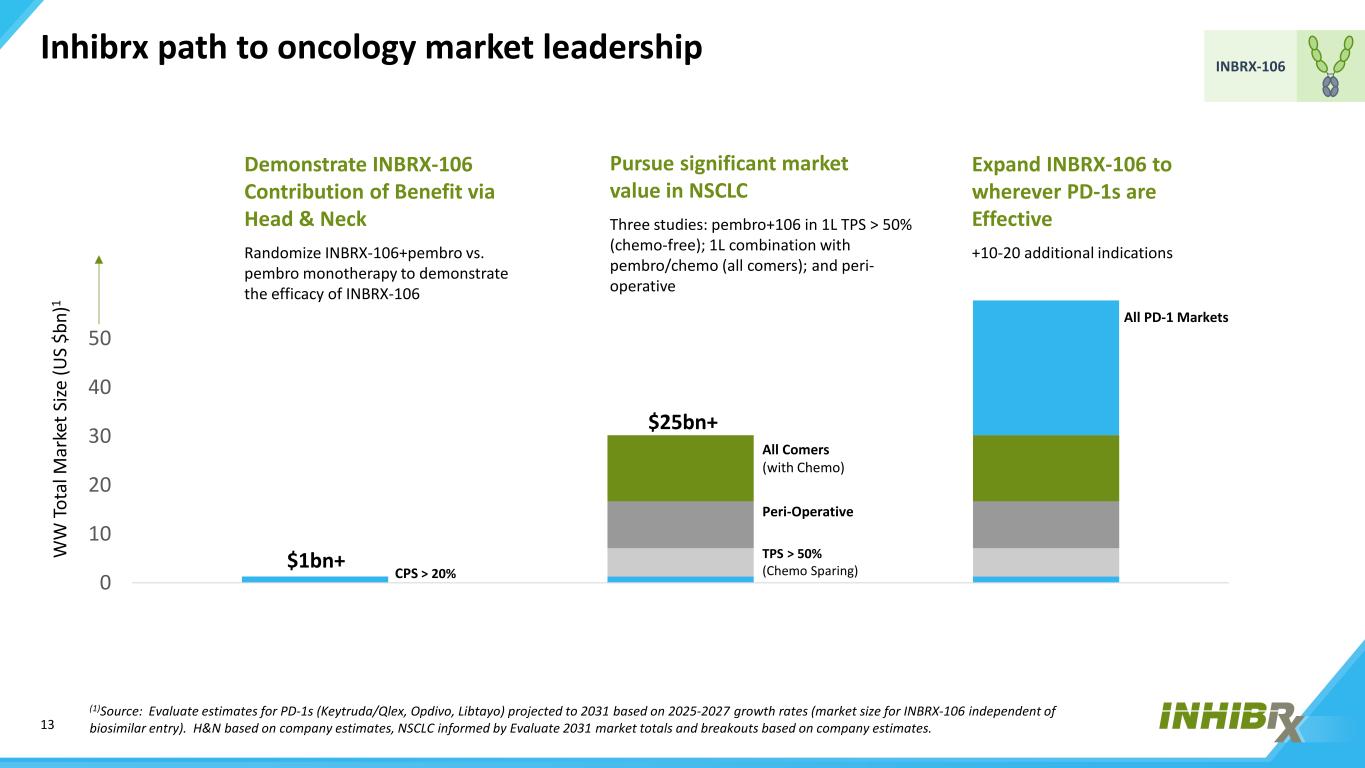
13 INBRX-106 Inhibrx path to oncology market leadership 0 10 20 30 40 50 60 70 CPS > 20% TPS > 50% (Chemo Sparing) Peri-Operative All Comers (with Chemo) All PD-1 Markets W W To ta l M ar ke t S ize (U S $b n) 1 (1)Source: Evaluate estimates for PD-1s (Keytruda/Qlex, Opdivo, Libtayo) projected to 2031 based on 2025-2027 growth rates (market size for INBRX-106 independent of biosimilar entry). H&N based on company estimates, NSCLC informed by Evaluate 2031 market totals and breakouts based on company estimates. $1bn+ $25bn+ $50bn+ Demonstrate INBRX-106 Contribution of Benefit via Head & Neck Randomize INBRX-106+pembro vs. pembro monotherapy to demonstrate the efficacy of INBRX-106 Pursue significant market value in NSCLC Three studies: pembro+106 in 1L TPS > 50% (chemo-free); 1L combination with pembro/chemo (all comers); and peri- operative Expand INBRX-106 to wherever PD-1s are Effective +10-20 additional indications
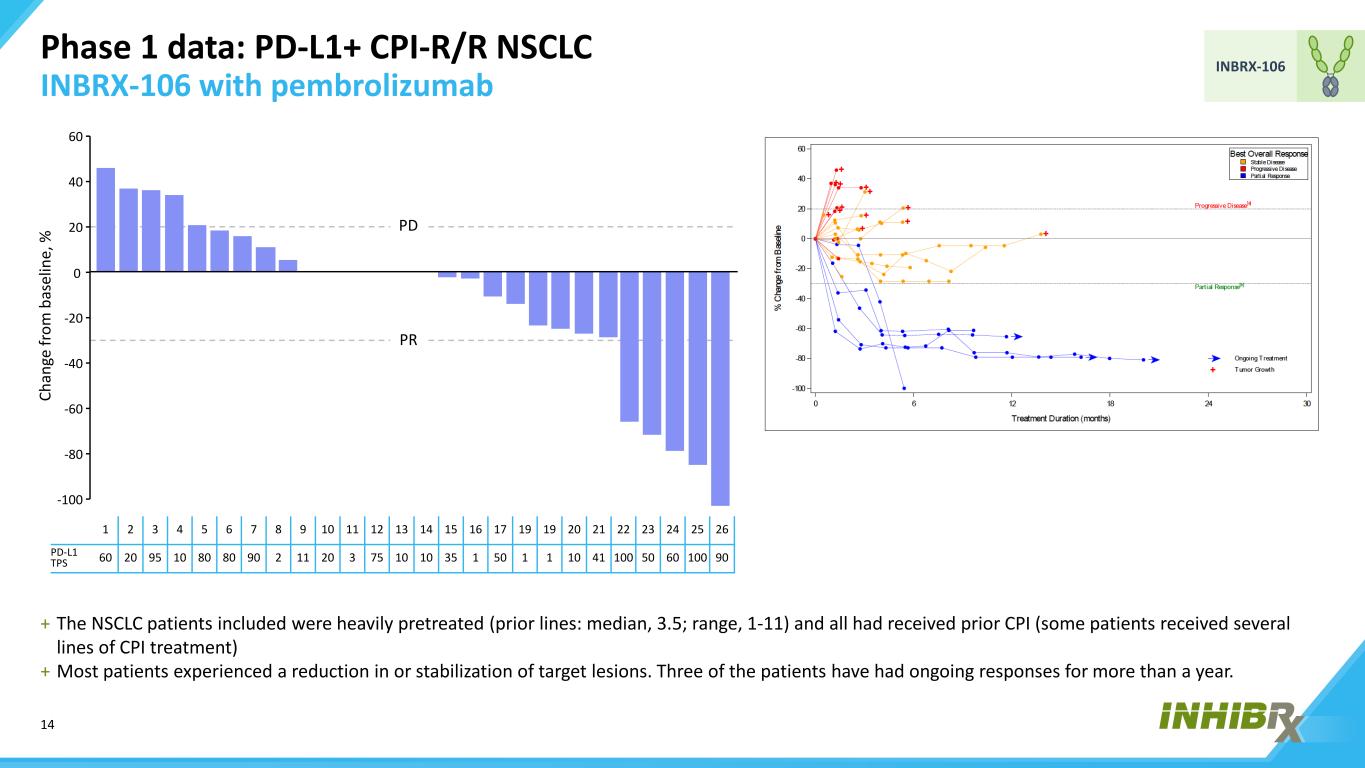
14 INBRX-106 Phase 1 data: PD-L1+ CPI-R/R NSCLC INBRX-106 with pembrolizumab 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 19 19 20 21 22 23 24 25 26 PD-L1 TPS 60 20 95 10 80 80 90 2 11 20 3 75 10 10 35 1 50 1 1 10 41 100 50 60 100 90 + The NSCLC patients included were heavily pretreated (prior lines: median, 3.5; range, 1-11) and all had received prior CPI (some patients received several lines of CPI treatment) + Most patients experienced a reduction in or stabilization of target lesions. Three of the patients have had ongoing responses for more than a year. Ch an ge fr om b as el in e, % 0 -100 -80 -60 -40 -20 20 60 40 PR PD
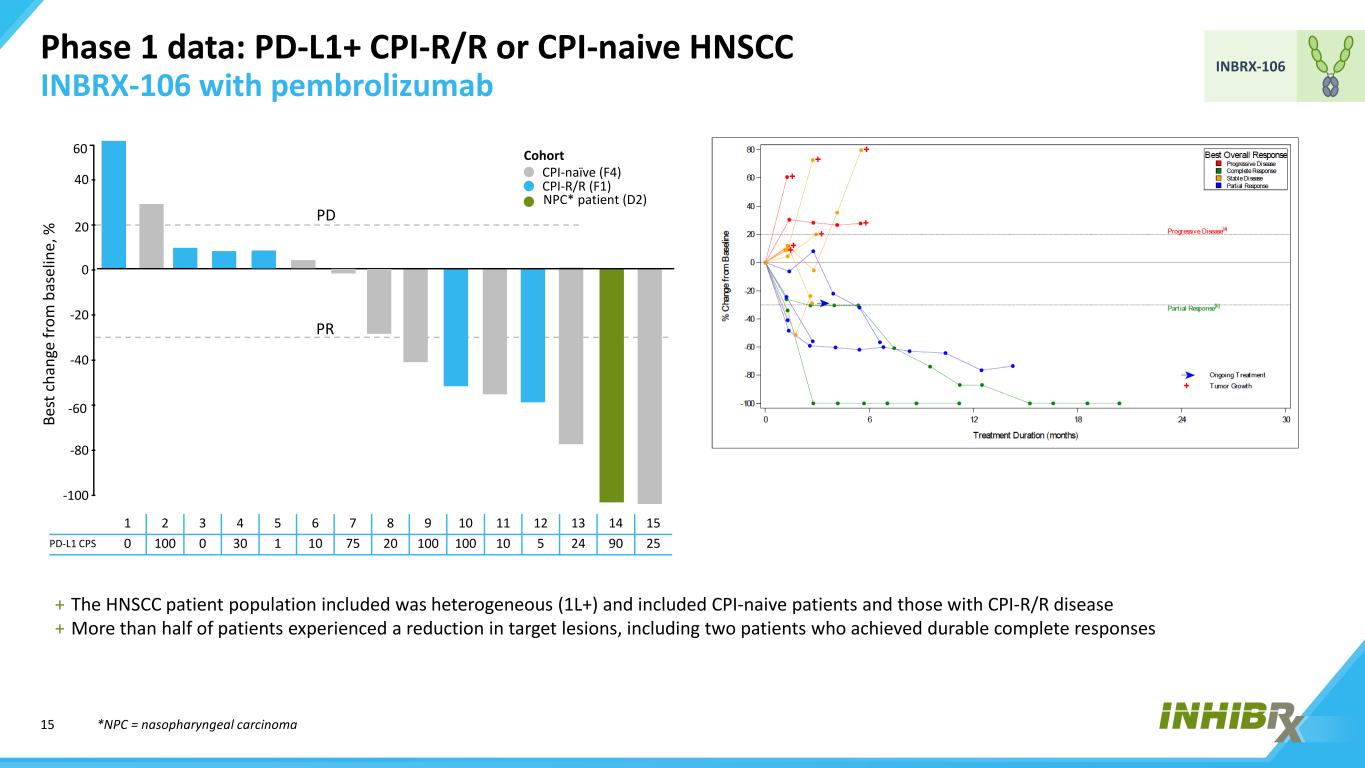
15 INBRX-106 Phase 1 data: PD-L1+ CPI-R/R or CPI-naive HNSCC INBRX-106 with pembrolizumab 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 PD-L1 CPS 0 100 0 30 1 10 75 20 100 100 10 5 24 90 25 + The HNSCC patient population included was heterogeneous (1L+) and included CPI-naive patients and those with CPI-R/R disease + More than half of patients experienced a reduction in target lesions, including two patients who achieved durable complete responses *NPC = nasopharyngeal carcinoma -60 PR PD NPC* patient (D2) Be st c ha ng e fr om b as el in e, % Cohort CPI-naïve (F4) CPI-R/R (F1) 20 -100 -80 -40 -20 0 40 60

ozekibart (INBRX-109) Selectively inducing apoptosis in tumor cells through tetravalent DR5 agonism
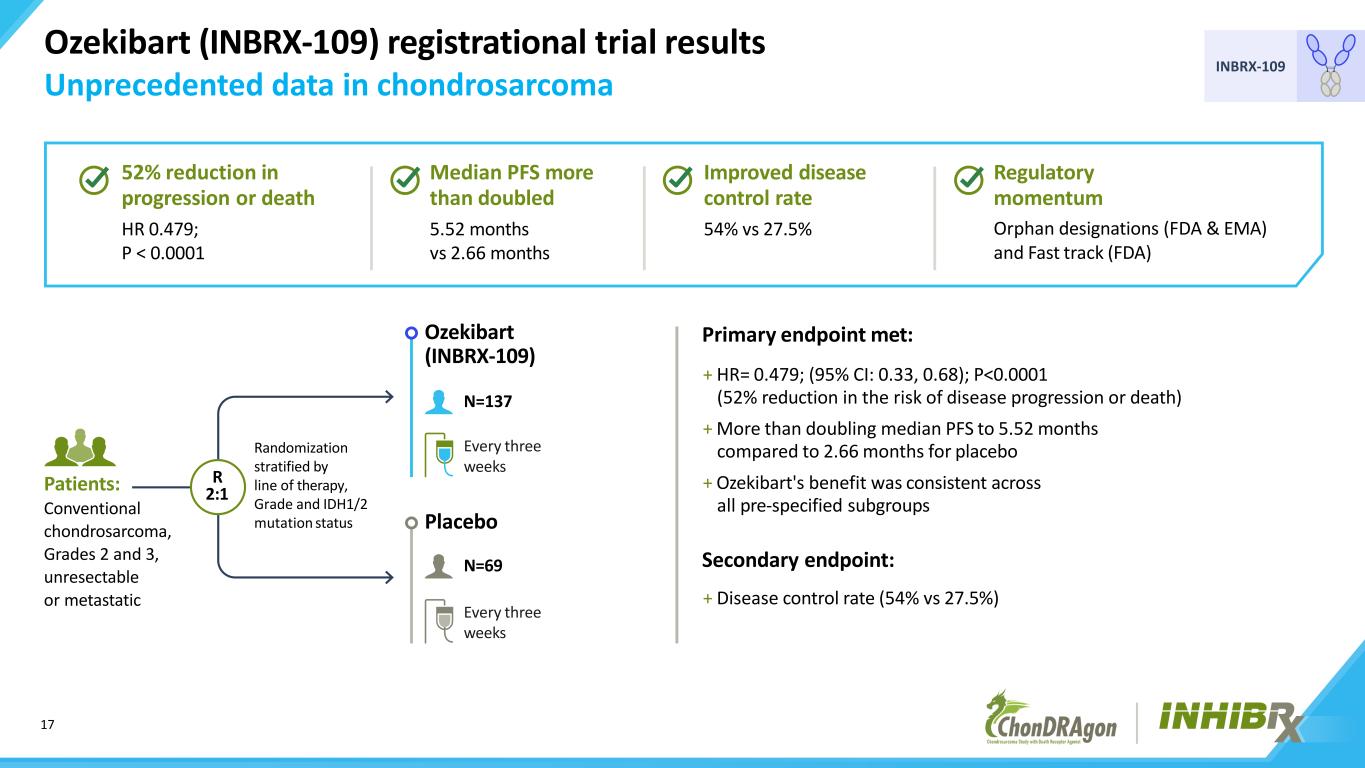
17 INBRX-109 Ozekibart (INBRX-109) registrational trial results Unprecedented data in chondrosarcoma Primary endpoint met: + HR= 0.479; (95% CI: 0.33, 0.68); P<0.0001 (52% reduction in the risk of disease progression or death) + More than doubling median PFS to 5.52 months compared to 2.66 months for placebo + Ozekibart's benefit was consistent across all pre-specified subgroups Secondary endpoint: + Disease control rate (54% vs 27.5%) Patients: Conventional chondrosarcoma, Grades 2 and 3, unresectable or metastatic R 2:1 Ozekibart (INBRX-109) Placebo Every three weeks Every three weeks N=137 N=69 Randomization stratified by line of therapy, Grade and IDH1/2 mutation status Regulatory momentum Orphan designations (FDA & EMA) and Fast track (FDA) Improved disease control rate 54% vs 27.5% Median PFS more than doubled 5.52 months vs 2.66 months 52% reduction in progression or death HR 0.479; P < 0.0001
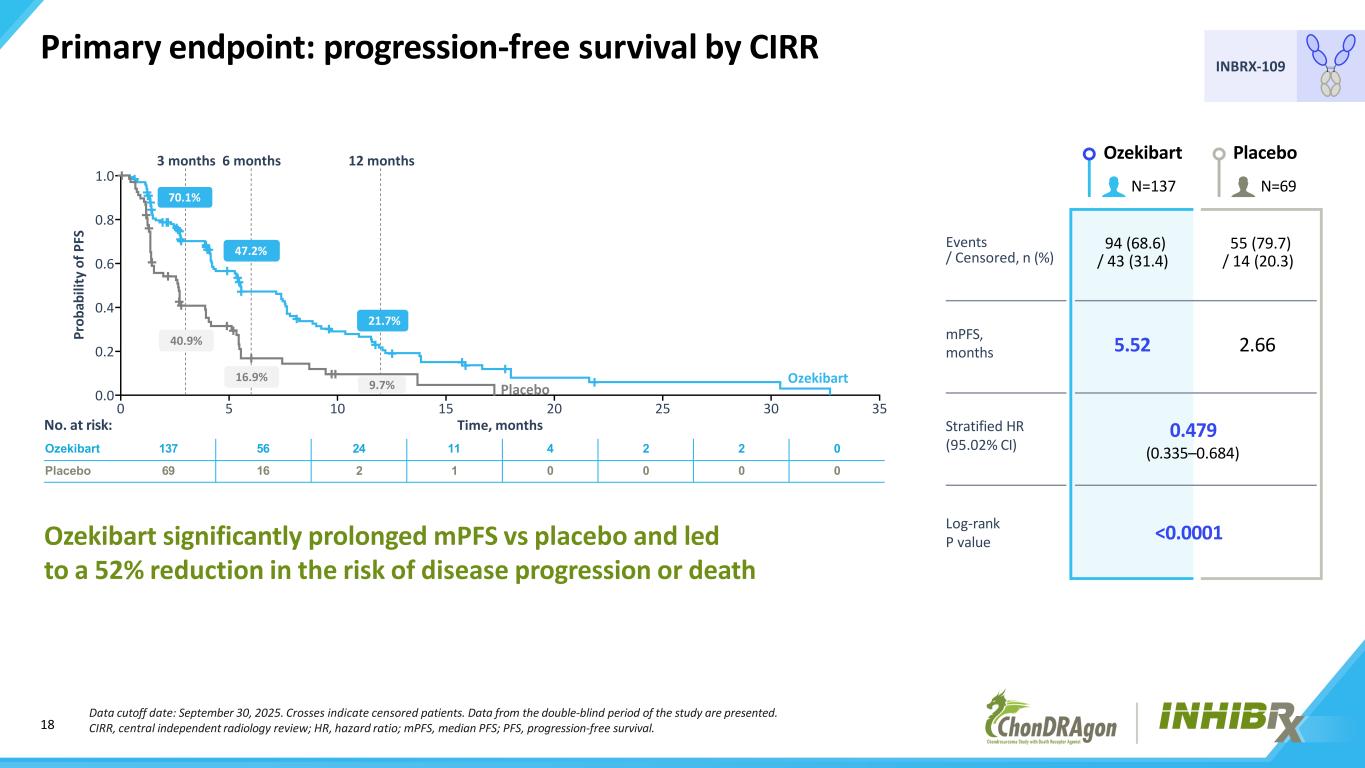
18 INBRX-109 Primary endpoint: progression-free survival by CIRR Data cutoff date: September 30, 2025. Crosses indicate censored patients. Data from the double-blind period of the study are presented. CIRR, central independent radiology review; HR, hazard ratio; mPFS, median PFS; PFS, progression-free survival. Ozekibart significantly prolonged mPFS vs placebo and led to a 52% reduction in the risk of disease progression or death Ozekibart Placebo 0.479 (0.335–0.684) <0.0001 5.52 2.66mPFS, months Stratified HR (95.02% CI) Log-rank P value Ozekibart 137 56 24 11 4 2 2 0 Placebo 69 16 2 1 0 0 0 0 No. at risk: Events / Censored, n (%) 94 (68.6) / 43 (31.4) 55 (79.7) / 14 (20.3) N=137 N=69 0 5 10 15 20 25 30 35 Time, months 0.0 0.2 0.4 0.6 0.8 1.0 Pr ob ab ili ty o f P FS 3 months 6 months 12 months Ozekibart Placebo 70.1% 21.7% 40.9% 16.9% 9.7% 47.2%
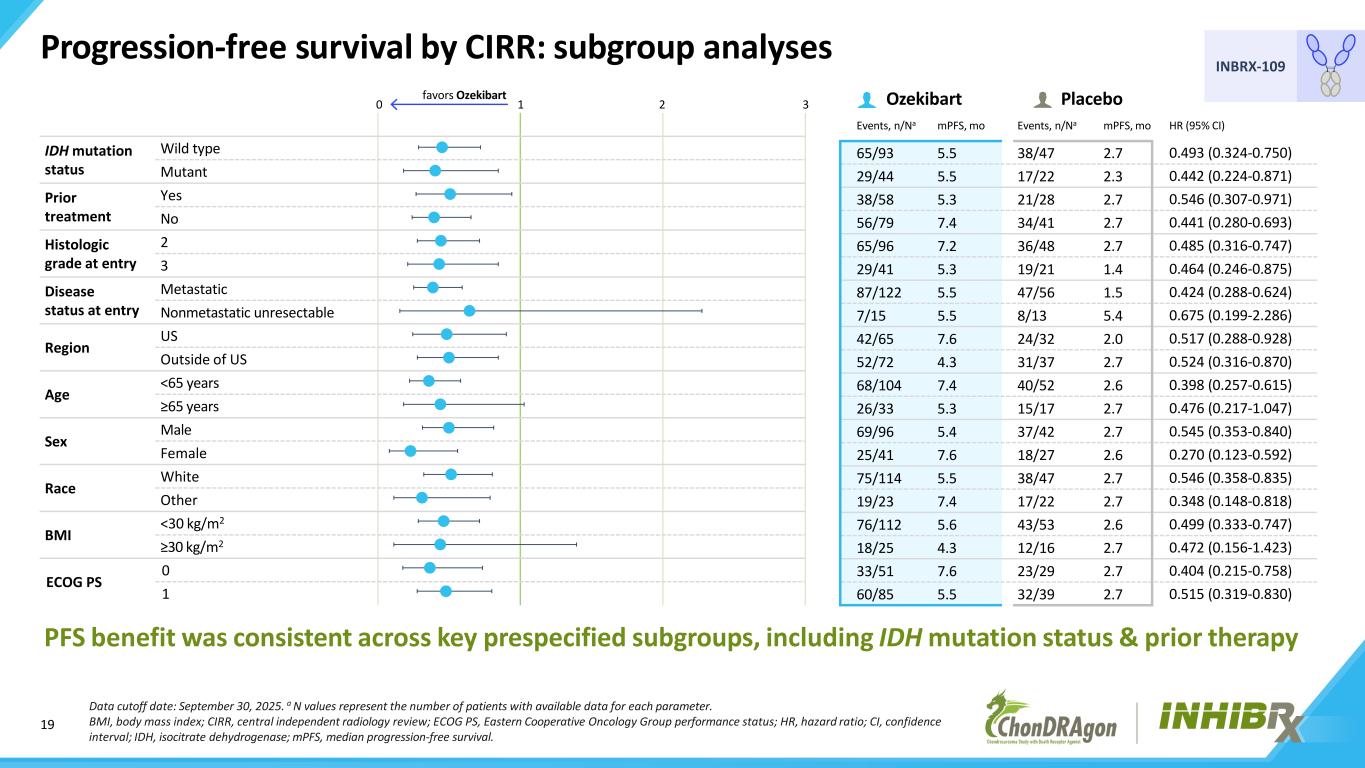
19 INBRX-109 IDH mutation status Wild type Mutant Prior treatment Yes No Histologic grade at entry 2 3 Disease status at entry Metastatic Nonmetastatic unresectable Region US Outside of US Age <65 years ≥65 years Sex Male Female Race White Other BMI <30 kg/m2 ≥30 kg/m2 ECOG PS 0 1 Progression-free survival by CIRR: subgroup analyses Data cutoff date: September 30, 2025. a N values represent the number of patients with available data for each parameter. BMI, body mass index; CIRR, central independent radiology review; ECOG PS, Eastern Cooperative Oncology Group performance status; HR, hazard ratio; CI, confidence interval; IDH, isocitrate dehydrogenase; mPFS, median progression-free survival. PFS benefit was consistent across key prespecified subgroups, including IDH mutation status & prior therapy favors Ozekibart 0 1 2 3 Ozekibart Placebo Events, n/Na mPFS, mo Events, n/Na mPFS, mo HR (95% CI) 65/93 5.5 38/47 2.7 0.493 (0.324-0.750) 29/44 5.5 17/22 2.3 0.442 (0.224-0.871) 38/58 5.3 21/28 2.7 0.546 (0.307-0.971) 56/79 7.4 34/41 2.7 0.441 (0.280-0.693) 65/96 7.2 36/48 2.7 0.485 (0.316-0.747) 29/41 5.3 19/21 1.4 0.464 (0.246-0.875) 87/122 5.5 47/56 1.5 0.424 (0.288-0.624) 7/15 5.5 8/13 5.4 0.675 (0.199-2.286) 42/65 7.6 24/32 2.0 0.517 (0.288-0.928) 52/72 4.3 31/37 2.7 0.524 (0.316-0.870) 68/104 7.4 40/52 2.6 0.398 (0.257-0.615) 26/33 5.3 15/17 2.7 0.476 (0.217-1.047) 69/96 5.4 37/42 2.7 0.545 (0.353-0.840) 25/41 7.6 18/27 2.6 0.270 (0.123-0.592) 75/114 5.5 38/47 2.7 0.546 (0.358-0.835) 19/23 7.4 17/22 2.7 0.348 (0.148-0.818) 76/112 5.6 43/53 2.6 0.499 (0.333-0.747) 18/25 4.3 12/16 2.7 0.472 (0.156-1.423) 33/51 7.6 23/29 2.7 0.404 (0.215-0.758) 60/85 5.5 32/39 2.7 0.515 (0.319-0.830)
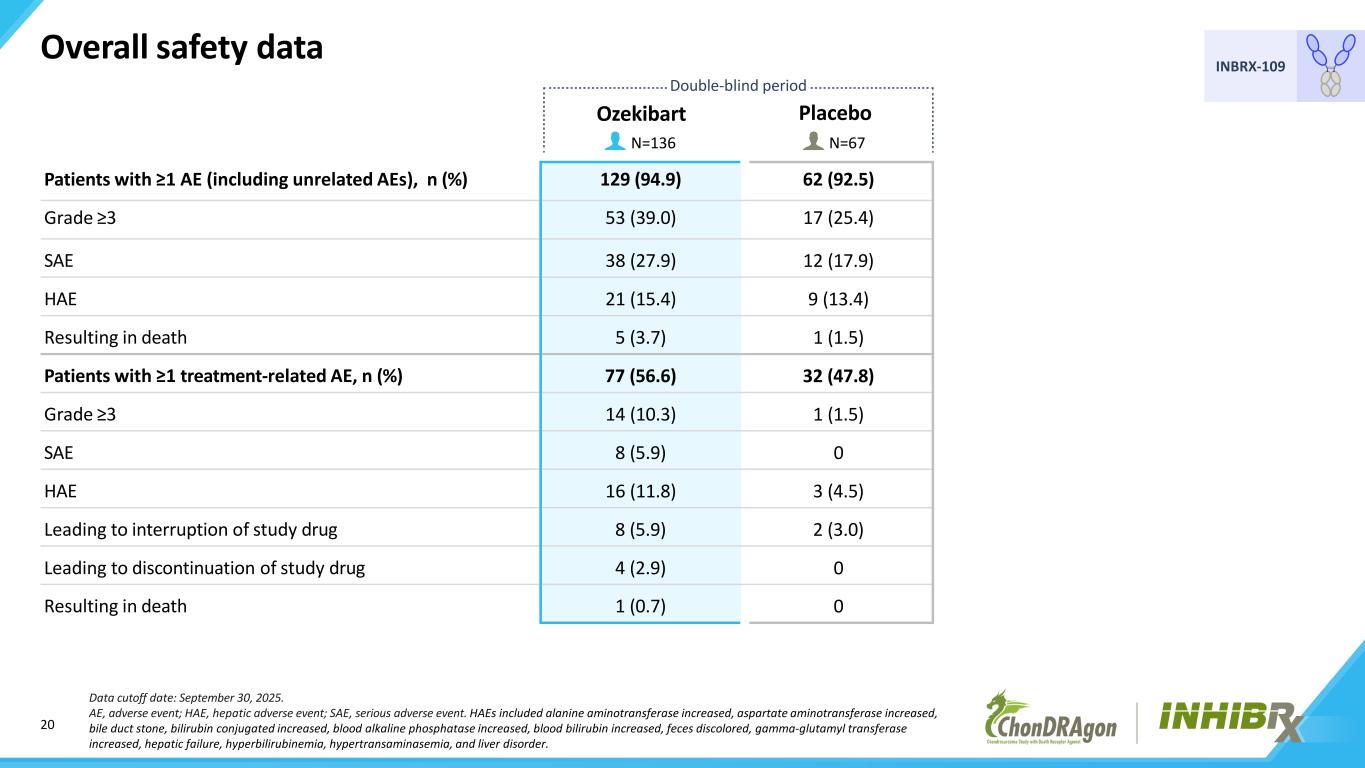
20 INBRX-109 Patients with ≥1 AE (including unrelated AEs), n (%) 129 (94.9) 62 (92.5) Grade ≥3 53 (39.0) 17 (25.4) SAE 38 (27.9) 12 (17.9) HAE 21 (15.4) 9 (13.4) Resulting in death 5 (3.7) 1 (1.5) Patients with ≥1 treatment-related AE, n (%) 77 (56.6) 32 (47.8) Grade ≥3 14 (10.3) 1 (1.5) SAE 8 (5.9) 0 HAE 16 (11.8) 3 (4.5) Leading to interruption of study drug 8 (5.9) 2 (3.0) Leading to discontinuation of study drug 4 (2.9) 0 Resulting in death 1 (0.7) 0 Overall safety data Placebo Data cutoff date: September 30, 2025. AE, adverse event; HAE, hepatic adverse event; SAE, serious adverse event. HAEs included alanine aminotransferase increased, aspartate aminotransferase increased, bile duct stone, bilirubin conjugated increased, blood alkaline phosphatase increased, blood bilirubin increased, feces discolored, gamma-glutamyl transferase increased, hepatic failure, hyperbilirubinemia, hypertransaminasemia, and liver disorder. Double-blind period Ozekibart N=136 N=67
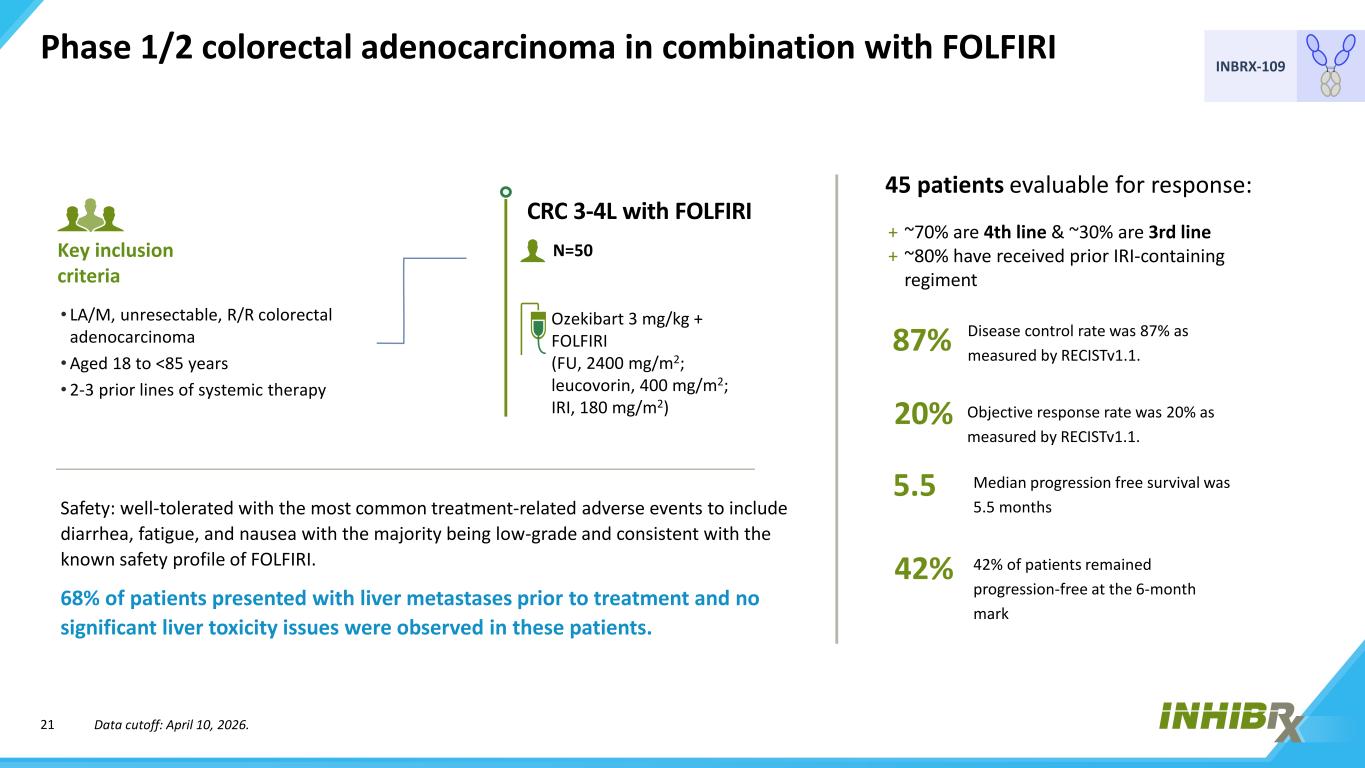
21 INBRX-109 Phase 1/2 colorectal adenocarcinoma in combination with FOLFIRI Safety: well-tolerated with the most common treatment-related adverse events to include diarrhea, fatigue, and nausea with the majority being low-grade and consistent with the known safety profile of FOLFIRI. 68% of patients presented with liver metastases prior to treatment and no significant liver toxicity issues were observed in these patients. + ~70% are 4th line & ~30% are 3rd line + ~80% have received prior IRI-containing regiment Disease control rate was 87% as measured by RECISTv1.1. 87% Objective response rate was 20% as measured by RECISTv1.1. 20% 45 patients evaluable for response: Median progression free survival was 5.5 months 5.5 42% of patients remained progression-free at the 6-month mark 42% Data cutoff: April 10, 2026. • LA/M, unresectable, R/R colorectal adenocarcinoma • Aged 18 to <85 years • 2-3 prior lines of systemic therapy Key inclusion criteria CRC 3-4L with FOLFIRI Ozekibart 3 mg/kg + FOLFIRI (FU, 2400 mg/m2; leucovorin, 400 mg/m2; IRI, 180 mg/m2) N=50
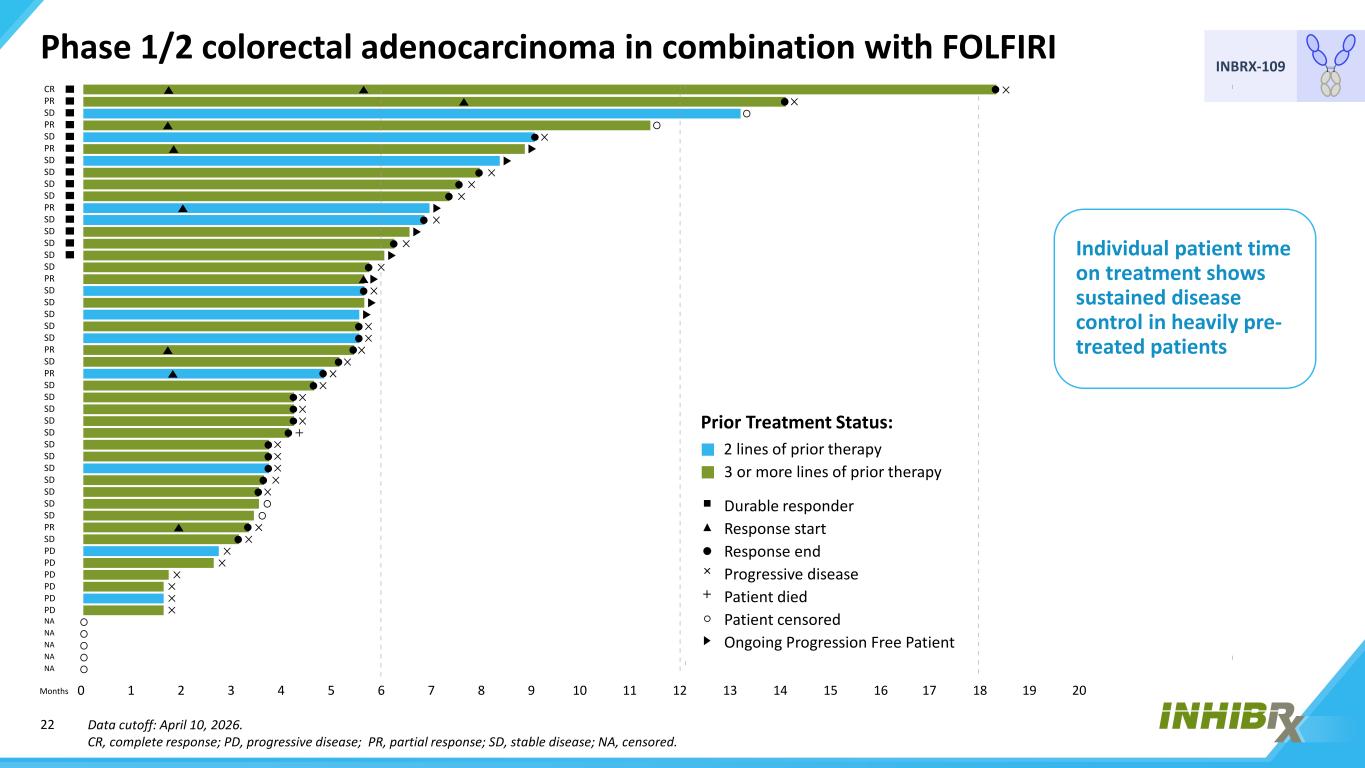
22 INBRX-109 Data cutoff: April 10, 2026. CR, complete response; PD, progressive disease; PR, partial response; SD, stable disease; NA, censored. Individual patient time on treatment shows sustained disease control in heavily pre- treated patients Phase 1/2 colorectal adenocarcinoma in combination with FOLFIRI 0 1 2 3 4 5 7 8 9 10 11 13 14 15 16 17 19 206 12 18 2 lines of prior therapy 3 or more lines of prior therapy Durable responder Response start Response end Progressive disease Patient died Patient censored Ongoing Progression Free Patient Prior Treatment Status: Months CR PR SD PR SD PR SD SD SD SD PR SD SD SD SD SD PR SD SD SD SD SD PR SD PR SD SD SD SD SD SD SD SD SD SD SD SD PR SD PD PD PD PD PD PD NA NA NA NA NA
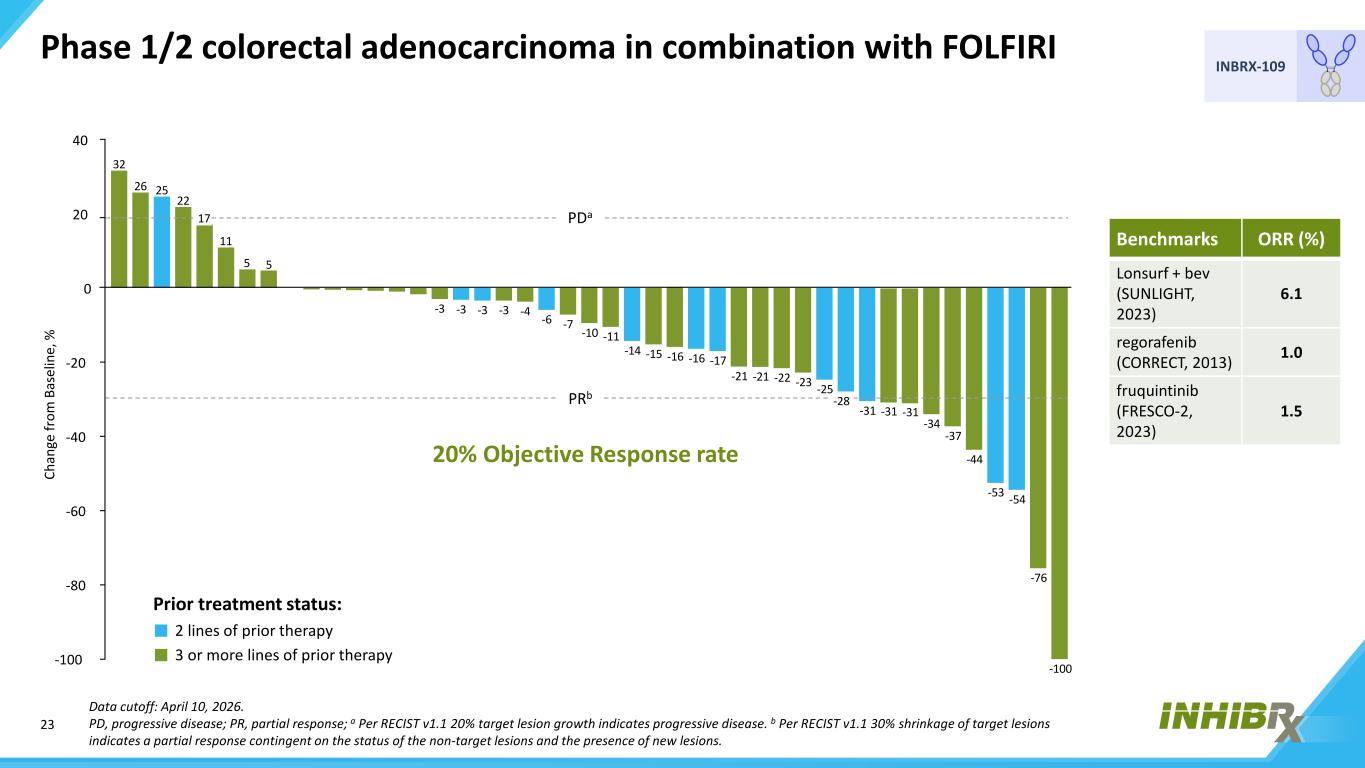
23 INBRX-109 Data cutoff: April 10, 2026. PD, progressive disease; PR, partial response; a Per RECIST v1.1 20% target lesion growth indicates progressive disease. b Per RECIST v1.1 30% shrinkage of target lesions indicates a partial response contingent on the status of the non-target lesions and the presence of new lesions. 40 20 0 -20 -40 -60 -80 -100 -100 -76 -54-53 -44 -37 -34 -31-31-31 -28 -25-23-22-21-21 -17-16-16-15-14 -11-10 -7-6 -4-3-3-3-3 55 11 17 22 2526 32 PDa PRb Ch an ge fr om B as el in e, % Prior treatment status: 2 lines of prior therapy 3 or more lines of prior therapy Phase 1/2 colorectal adenocarcinoma in combination with FOLFIRI Benchmarks ORR (%) Lonsurf + bev (SUNLIGHT, 2023) 6.1 regorafenib (CORRECT, 2013) 1.0 fruquintinib (FRESCO-2, 2023) 1.5 20% Objective Response rate
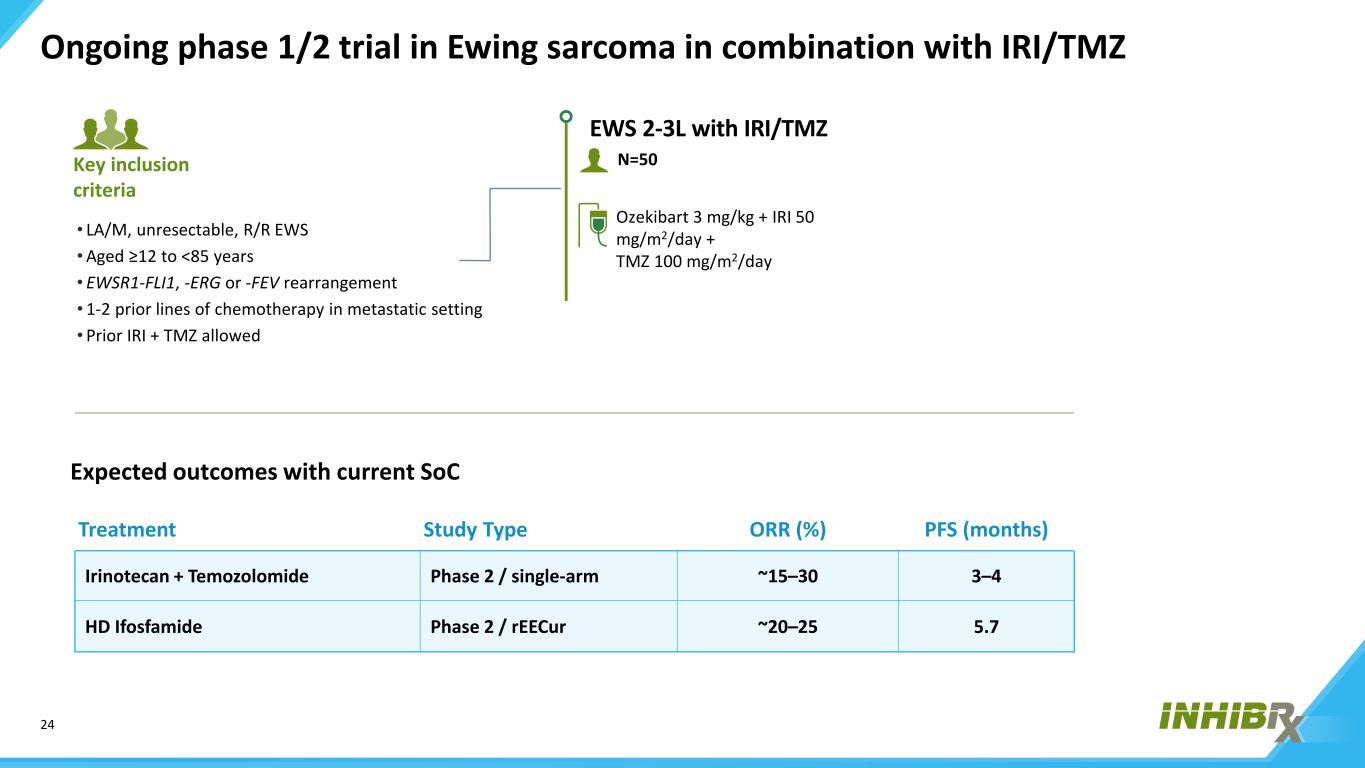

24 INBRX-109 Ongoing phase 1/2 trial in Ewing sarcoma in combination with IRI/TMZ • LA/M, unresectable, R/R EWS • Aged ≥12 to <85 years • EWSR1-FLI1, -ERG or -FEV rearrangement • 1-2 prior lines of chemotherapy in metastatic setting • Prior IRI + TMZ allowed Key inclusion criteria EWS 2-3L with IRI/TMZ Ozekibart 3 mg/kg + IRI 50 mg/m2/day + TMZ 100 mg/m2/day N=50 Expected outcomes with current SoC Treatment Study Type ORR (%) PFS (months) Irinotecan + Temozolomide Phase 2 / single-arm ~15–30 3–4 HD Ifosfamide Phase 2 / rEECur ~20–25 5.7
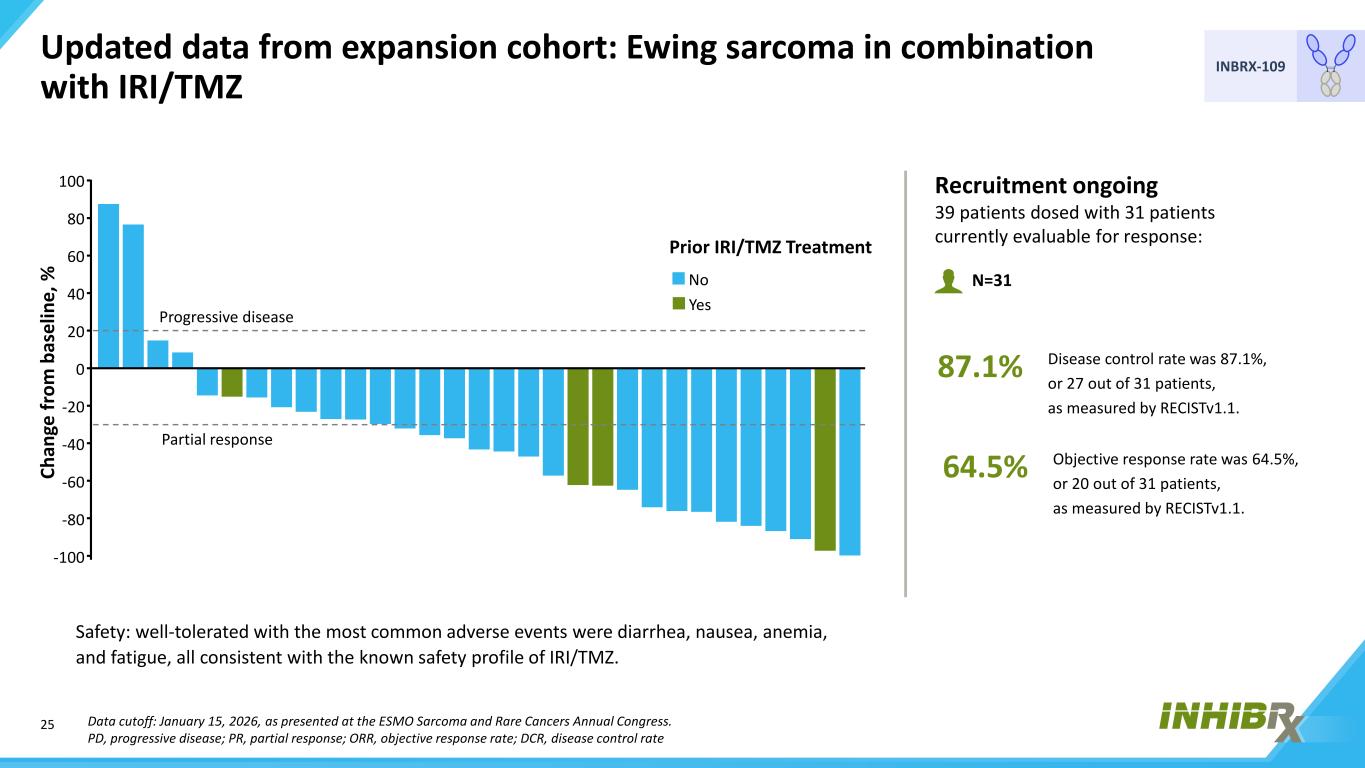
25 INBRX-109 Updated data from expansion cohort: Ewing sarcoma in combination with IRI/TMZ Data cutoff: January 15, 2026, as presented at the ESMO Sarcoma and Rare Cancers Annual Congress. PD, progressive disease; PR, partial response; ORR, objective response rate; DCR, disease control rate Recruitment ongoing 39 patients dosed with 31 patients currently evaluable for response: N=31 Disease control rate was 87.1%, or 27 out of 31 patients, as measured by RECISTv1.1. 87.1% Objective response rate was 64.5%, or 20 out of 31 patients, as measured by RECISTv1.1. 64.5% Safety: well-tolerated with the most common adverse events were diarrhea, nausea, anemia, and fatigue, all consistent with the known safety profile of IRI/TMZ. 100 60 0 -40 -100 Ch an ge fr om b as el in e, % 80 40 20 -20 -60 -80 Progressive disease Partial response Prior IRI/TMZ Treatment No Yes
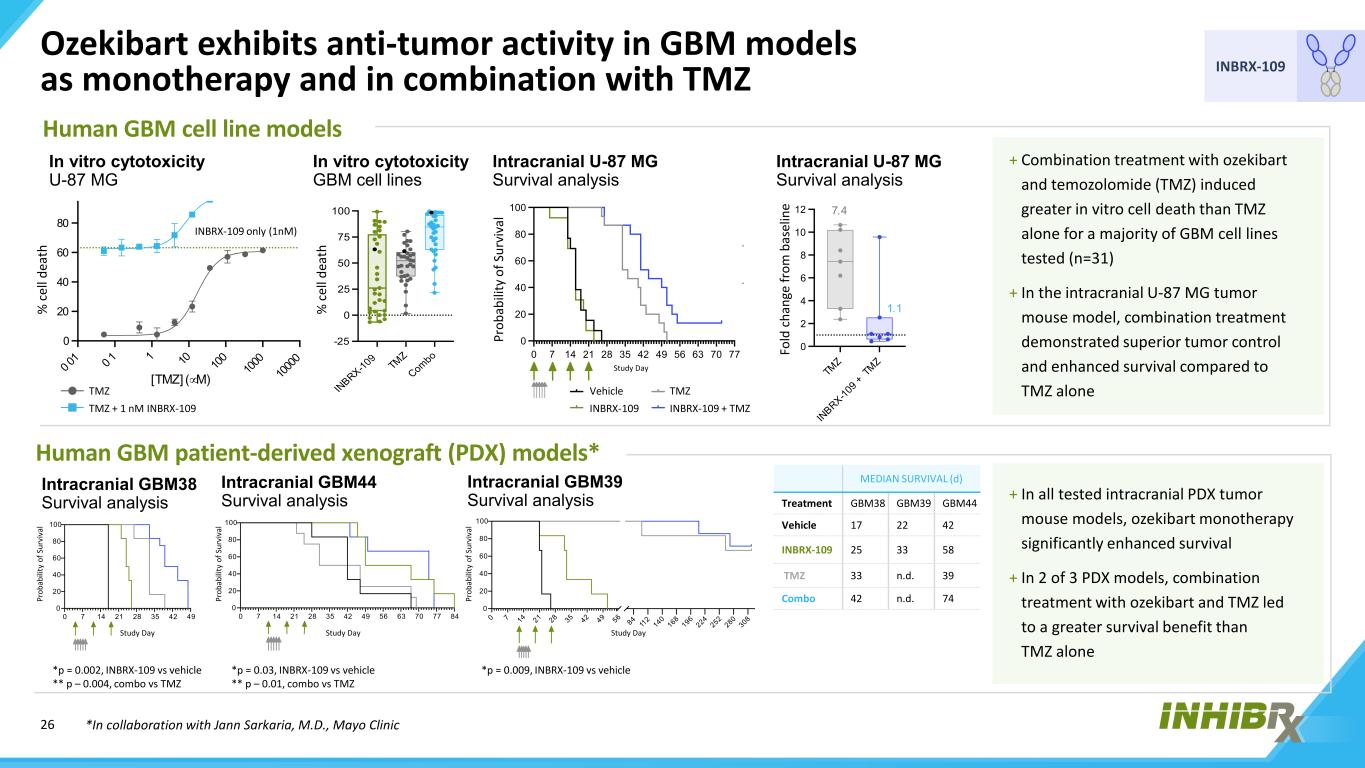
26 INBRX-109 0 7 14 21 28 35 42 49 0 20 40 60 80 100 0 20 40 60 80 100 0 7 14 21 28 35 42 49 56 63 70 77 84 0 20 40 60 80 100 y 0 2 4 6 8 10 12 7.4 1.1 0 7 14 21 28 35 42 49 56 63 70 77 0 20 40 60 80 100 Vehicle INBRX-1 TMZ INBRX-1 -25 0 25 50 75 100 0 20 40 60 80 [TMZ] (∝M) Ozekibart exhibits anti-tumor activity in GBM models as monotherapy and in combination with TMZ In vitro cytotoxicity GBM cell lines + In all tested intracranial PDX tumor mouse models, ozekibart monotherapy significantly enhanced survival + In 2 of 3 PDX models, combination treatment with ozekibart and TMZ led to a greater survival benefit than TMZ alone In vitro cytotoxicity U-87 MG INBRX-109 only (1nM) Intracranial U-87 MG Survival analysis Intracranial U-87 MG Survival analysis + Combination treatment with ozekibart and temozolomide (TMZ) induced greater in vitro cell death than TMZ alone for a majority of GBM cell lines tested (n=31) + In the intracranial U-87 MG tumor mouse model, combination treatment demonstrated superior tumor control and enhanced survival compared to TMZ alone Human GBM cell line models Human GBM patient-derived xenograft (PDX) models* Intracranial GBM44 Survival analysis Intracranial GBM38 Survival analysis Intracranial GBM39 Survival analysis *p = 0.002, INBRX-109 vs vehicle ** p – 0.004, combo vs TMZ *p = 0.03, INBRX-109 vs vehicle ** p – 0.01, combo vs TMZ *p = 0.009, INBRX-109 vs vehicle *In collaboration with Jann Sarkaria, M.D., Mayo Clinic % c el l d ea th % c el l d ea th Pr ob ab ili ty o f S ur vi va l Fo ld c ha ng e fr om b as el in e Pr ob ab ili ty o f S ur vi va l Pr ob ab ili ty o f S ur vi va l Pr ob ab ili ty o f S ur vi va l Study Day Study DayStudy Day MEDIAN SURVIVAL (d) Treatment GBM38 GBM39 GBM44 Vehicle 17 22 42 INBRX-109 25 33 58 TMZ 33 n.d. 39 Combo 42 n.d. 74 Study Day TMZ + 1 nM INBRX-109 TMZ INBRX-109 Vehicle INBRX-109 + TMZ TMZ

Investor Relations: KELLY DECK, CPA CFO 11025 N. Torrey Pines Road Suite 140 La Jolla, CA 92037 858.795.4260 ir@inhibrx.com